In a world divided by the Cold War, the Almaty declaration of 1978 was a triumph for humanity, write Anis Chowdhury and Jomo Kwame Sundaram. Then came the 1980s.
Anis Chowdhury and Jomo Kwame Sundaram
in Sydney and Kuala Lumpur
Inter Press Service

 Instead of a health system striving to provide universal healthcare, a fragmented, profit-driven market “non-system” has emerged. The 1980s’ neo-liberal counter-revolution against the historic 1978 Alma-Ata Declaration is responsible.
Instead of a health system striving to provide universal healthcare, a fragmented, profit-driven market “non-system” has emerged. The 1980s’ neo-liberal counter-revolution against the historic 1978 Alma-Ata Declaration is responsible.
Neoliberal health reforms over the last four decades have reversed progress made at the World Health Organization (WHO) Assembly in the capital of the then Socialist Republic of Kazakhstan, now known as Almaty.
Then, 134 WHO member states reached a historic consensus reaffirming health as a human right. It recognized that heath is determined by environmental, socio-economic and political conditions, not only medical factors narrowly understood.
The declaration stated,
“Governments have a responsibility for the health of their people which can be fulfilled only by the provision of adequate health and social measures.”
Also:
“The people have the right and duty to participate individually and collectively in the planning and implementation of their health care.”
Countries committed to the fundamental right of every human being to enjoy the highest attainable standard of healthcare without discrimination. They agreed that primary healthcare is key to addressing crucial determinants of health.

International conference on primary health care in Almaty, 1978. (CC BY-SA 3.0, Wikimedia Commons)
Alma-Ata eschewed overly hospital-centric and medicalized systems, instead favoring a more social approach to medicine. In a world divided by the Cold War, the declaration was a triumph for humanity, promising progress for global health.
It recognized the crucial contributions of multilateral cooperation, peace, social health determinants, health equity norms, community participation in planning, implementation and regulation, and involving other ‘sectors’ to promote health.
Primary Healthcare
Some developing countries — e.g., China, Costa Rica, Cuba and Sri Lanka — had already achieved impressive health outcomes at relatively low cost, raising life expectancy by 15 to 20 years in under two decades.
Instead of just curative medicine and clinical care, prevention and public health were given more emphasis. Basic health services, improved diets, safe water, better sanitation, health education and disease prevention became central to such initiatives.
Mainly rural community health workers were trained to help communities address common health problems. Differences in national government approaches, contexts and needs have also shaped primary healthcare outcomes, reach and efficacy, e.g., in delivering healthcare to the poor.
Despite reversals elsewhere, some efforts have continued, even expanded. Even in the 21st century, large-scale primary healthcare efforts have made remarkable health gains, e.g., Brazil’s Programa Saude da Familia and Thailand’s Universal Coverage Scheme.
Lalonde Report Turning Point
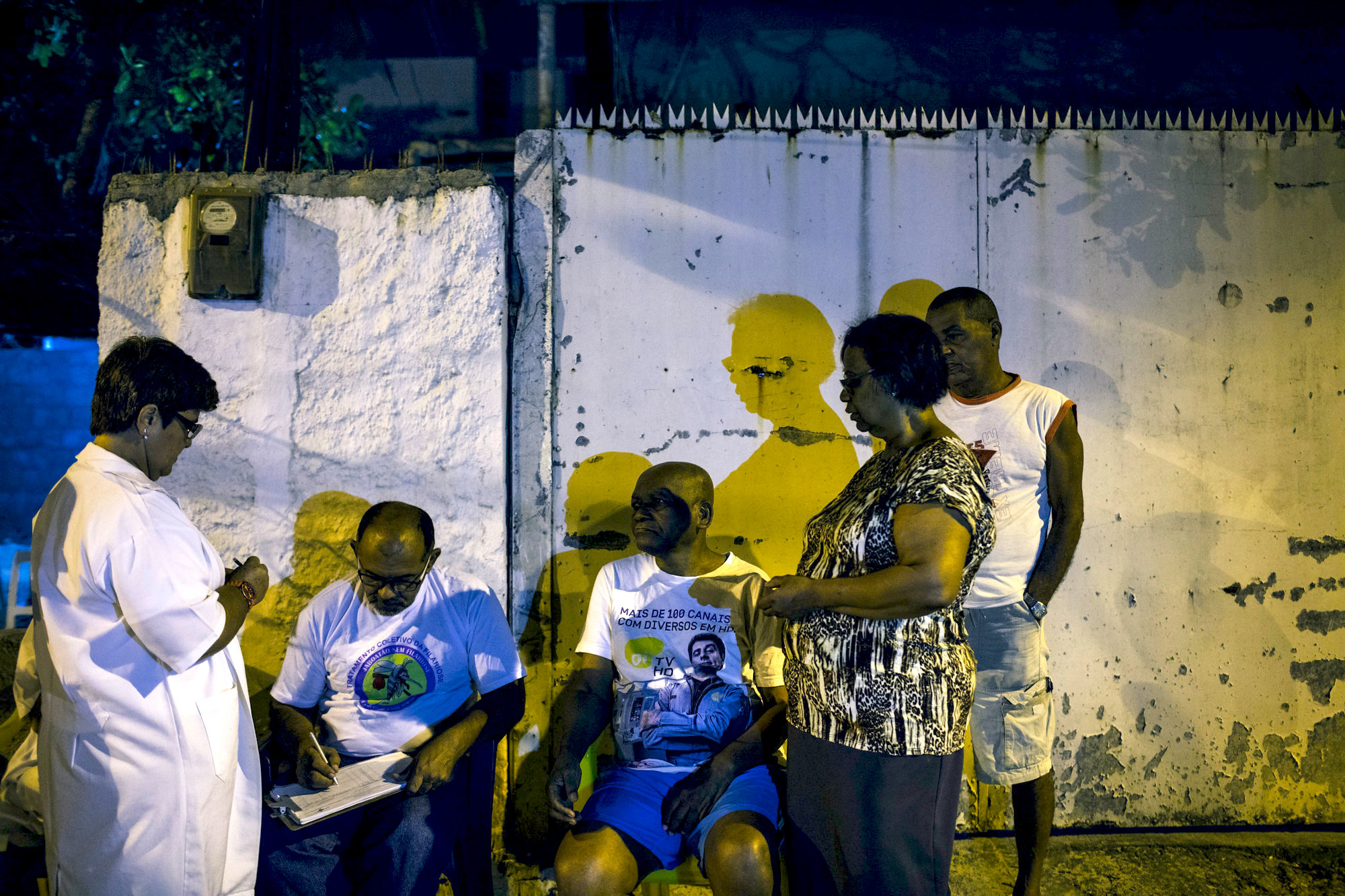
2015: Community health workers administering the microfilaria test — which must be conducted between 11 p.m. and 1 a.m. — outside a bar in Pernambuco, Brazil, (Pan American Health Organization, Flickr, CC BY-NC 2.0)
Alma-Ata inverted health policy priorities, as 90 perecent of health problems were recognized as due to lifestyles, environments and human biology, with only 10 percent due to the “healthcare system,” as noted by Canada’s 1974 Lalonde Report.
The Lalonde Report reaffirmed WHO’s basic approach.
Its 1946 constitution had affirmed, “Health is a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity.”
The report’s multidimensional approach to human health marked a turning point, reshaping policy approaches. Similar health assessments, with more holistic understandings, were also influential.
Reports from the U.K., U.S., Sweden and elsewhere also challenged the dominant medicalized approach to healthcare promoted by big pharmaceutical and other health-related businesses.
Neoliberal Ascendance
Developments since the 1980s have set back and reversed the Alma-Ata commitments. Latin American and other debt crises paved the way for the neo-liberal “Washington Consensus” counter-revolution.
“Rescue packages” from the International Monetary Fund and World Bank, especially structural adjustment programs (SAPs), demanded public spending cuts. These reduced social spending, cutting funding for health.
Thus, many primary healthcare programs, including community health workers, did not last.
Citing cost recovery, structural adjustment programs pressed to impose user fees and privatize health services. The outcomes betrayed Alma-Ata’s promise of greater health equity, and “health for all” by 2000, undermining prospects for universal health coverage.
The World Bank’s 1993 World Development Report, “Investing in Health,” also undermined Alma-Ata. Justifying state healthcare provisioning cuts, it promoted for-profit health financing and other private solutions.
Healthcare Financing Key

Bill and Melinda Gates Foundation in Seattle. (Adbar, CC BY-SA 3.0, Wikimedia Commons)
In neoliberal dialect, strengthening health systems meant “enhancing public-private partnerships” among other such interventions. The Bank provided substantial financial support to fund its recommendations.
Despite Alma-Ata, the WHO’s 2000 World Health Report criticized developing countries for “focusing on the public sector and often disregarding the — frequently much larger — private provision of care.” It argued, “Health policy and strategies need to cover the private provision of services and private financing.”
Addressing health progress became more “siloed” with the UN’s Millennium Development Goals (MDGs) indicators’ focus on curing and preventing particular diseases. Neither the WHO’s 2000 report nor the Millennium Development Goals reiterated Alma-Ata’s emphasis on social justice, equity and community participation.
Instead, that era saw more healthcare privatization, public-private partnerships and contracting out of services. After this neoliberal eclipse, WHO’s attempted U-turn, starting over a decade ago, has emphasized universal health care and socio-economic determinants, but the Alma-Ata betrayals prevail.
Thus, the Bank’s International Finance Corporation has been promoting private investments in healthcare services and infrastructure. Deploying billions, it buys public policy influence in Africa, India and beyond.
Philanthropy Rules
Unsurprisingly, cash-strapped governments have welcomed financial support from supposed “do-gooder” philanthropists. Many states have to cope with fragile, even crumbling health systems, often overwhelmed by old killers and new epidemics.
Such MDGs-inspired support has typically been via “vertical funds” targeting specific diseases – contrary to Alma-Ata. With more money than WHO’s paltry budget, corporate philanthropy has been remaking policies the world over.
Thus, the policy and ideological prejudices of the Gates Foundation; Gavi, Vaccine Alliance; Global Fund to Fight AIDS, Tuberculosis and Malaria have obscured Alma-Ata, also reshaping national health priorities.
Covid-19 has unveiled some more effects of various profit-driven healthcare inequities, chronic under-investment in primary healthcare and over-investment in profit-driven healthcare. They have not only hastened the retreat from “health for all” and universal healthcare, but also made the world more vulnerable to epidemics.
Worse, the interests and priorities of corporate philanthropy have not only raised the costs of, and thus delayed containing the pandemic, but also reversed much of the modest and uneven progress of recent decades, besides worsening inequalities.
Anis Chowdhury is adjunct professor at Western Sydney University and the University of New South Wales (Australia). He has held senior United Nations positions in New York and Bangkok.
Jomo Kwame Sundaram, a former economics professor, was United Nations assistant secretary-general for economic development, and received the Wassily Leontief Prize for Advancing the Frontiers of Economic Thought in 2007.
The views expressed are solely those of the authors and may or may not reflect those of Consortium News.

The idea of commodifying health care as though it were just another “thing” to buy at inflated cost is inhuman and socially devastating. Capitalism has nothing to offer society as a whole. It only entrenches the personal obscene wealth of a hand full of oligarchs and tramples the rest of the population into the dust. The actions of the ruling corporate elites is a death sentence for humanity and also for the planet Earth. Unless we the people can rise up and overthrow this monster, we are doomed to extinction.
Thanks to gates and many other zillionaires Amerika and the world care is hurry up a die. Sad