Brazilian health expert Margareth Dalcolmo says Covid-19-induced mortality has a social component that cannot be ignored — people are dying because they are poor.
Margareth Dalcolmo
interviewed by Christoph Heuser and Daniel Kopp
International Politics and Society
Christoph Heuser and Daniel Kopp: Brazil now accounts for more than a quarter of global deaths, with far above 3,000 deaths per day. Washington University is even forecasting 100,000 deaths in April alone. All the while, the Brazilian health system is on the brink of collapse. How did the pandemic get so out of control here?
 We have to understand the dynamics of the pandemic in Brazil. Covid-19 arrived here after carnival last year. We quickly understood that it was serious because it was an illness with a reproduction rate above one, a sign that the virus was highly transmissible. We learned that it was not just an atypical pneumonia but a systemic illness. In March, we started to have the first deaths amongst elderly and understand the risk factors. All this was part of an intense and deep learning curve.
We have to understand the dynamics of the pandemic in Brazil. Covid-19 arrived here after carnival last year. We quickly understood that it was serious because it was an illness with a reproduction rate above one, a sign that the virus was highly transmissible. We learned that it was not just an atypical pneumonia but a systemic illness. In March, we started to have the first deaths amongst elderly and understand the risk factors. All this was part of an intense and deep learning curve.
However, from the very beginning, we also witnessed a serious antagonism between the medical and scientific discourse and the federal government. That did a great disservice to the Brazilian population because the government denied the severity of the pandemic, the instructions that we as medical professionals tried to convey to the population, and the need for assistance to the underprivileged layers of the Brazilian population, since Brazil has a population of 13 million people that live in Favelas.
In fact, I was part of the group to provide support to Health Minister Luiz Henrique Mandetta in March last year. But right after that he was fired and left the Ministry of Health, we were never able to create harmony between politics and science again. This tension has been there almost since the very beginning and lasts until today. It’s not at all helpful. On the contrary, it makes the pandemic worse.
My immediate projection is very pessimistic. I previously said that we would have the saddest March in our lives and we had it. I think April will be even worse, and only in May things have a possibility to improve.
What role did political decisions play in creating this situation?

Brazil’s President Jair Bolsonaro, at right, with U.S. President Donald Trump at the White House, March 19. 2019. (Alan Santos, Palácio do Planalto, CC BY 2.0, Wikimedia Commons)
When the pandemic peaked in the southeast of Brazil, it was clear that Brazil was wasting time and energy discussing treatments that the medical literature had already demonstrated did not work. The government invested a good amount of money in buying chloroquine produced by the official laboratory, which it received from the U.S. Back then, President Donald Trump unloaded chloroquine in Brazil because it was banned over there.
In parallel, and that’s part of the Brazilian paradox, the country was prepared for the development of good Phase 3 studies for vaccines: CoronaVac, AstraZeneca, Pfizer and Johnson. But we made another major mistake as we didn’t negotiate in time to receive vaccines from manufacturers that were developing their high-quality Phase 3 studies here. It’s a fact that Pfizer offered vaccines to Brazil, and Brazil did not negotiate.
Every year, we vaccinate 80 million people with the flu shot, and we do it in six weeks — that’s more than 2 million shots a day. But we are not vaccinating right now, because we don’t have enough vaccines. We made mistakes in the negotiations, diplomatic mistakes vis-à-vis China, even though we have a technical cooperation in a contract with China, the active pharmaceutical ingredients (APIs) were delayed.
The Brazilian mutations of the virus, like the P1 first detected in Japan from a family coming from the Amazonian region, are a major concern in Europe and internationally. How dangerous is it for the region and beyond?
P1 isn’t more dangerous than the U.K. or the South African mutations. There are three identified so-called concerning variants at the moment. There is also the P2 strain, and now the variant that was detected in Bauru, a municipality in São Paulo, which is very similar to the South African mutation. Will we have others? Possibly yes. SARS-COV2 is not a highly mutating virus, but it does mutate like all viruses do. There are so far more than 400 mutations already detected, but most aren’t concerning.
The P1 strain is very transmissible. That’s why the profile of the disease changed in Brazil. We have already vaccinated a high proportion of the elderly population, so we can already see a 70 percent reduction in the rate of hospitalizations among the elderly. Now, we have a different profile made up of young people becoming ill. This means that the strain is more transmissible, and the population is leaving their homes more often. If you look at the average age of the people who are hospitalized, it’s much lower. A lot of people are under 50.
Of course, Brazil needs to vaccinate and contain the pandemic also because of international concerns. But we have our own concerns about the variants coming from other countries as well. We are enormously concerned about the South African variant because the AstraZeneca vaccine doesn’t offer protection against it. We are less worried about the U.K. variant, as it can be controlled with the AstraZeneca vaccine.
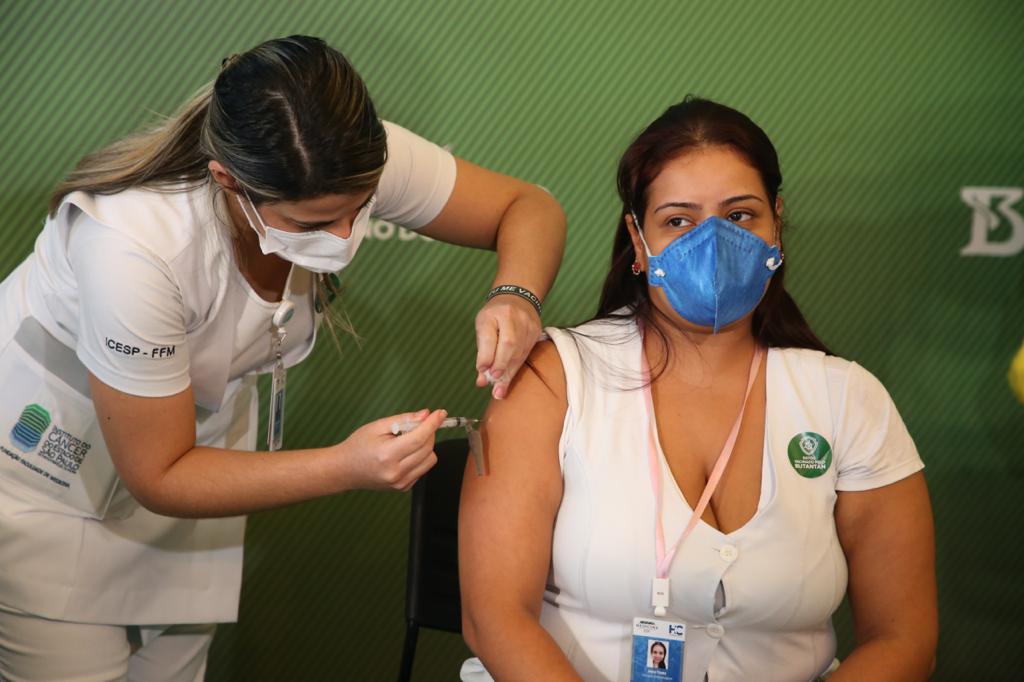
Covid-19 vaccination administered in Sao Paolo; Sinovac Coronavac (Brazilian version manufactured by Butantan Institute), January 2021. (Governo do Estado de São Paulo, CC BY 2.0, Wikimedia Commons)
Considering the infrastructure of the health system, do you think Brazil was well-prepared for the pandemic?
Brazil had two major weapons to confront the pandemic, which were our public health services (SUS) and social distancing. SUS is an extremely well-conceived system governed by the constitution — health care is a duty of the state and a right for all citizens that has to be free of charge, equitable and universal — and with state funding. But it has been underfunded for a certain number of years, with difficulties getting resources to already fragile populations. That’s why SUS was somewhat caught off guard. In such a situation, many states even had a sort of disintegration of SUS. For example, in state of Rio de Janeiro, the last mayor had dismantled the family care clinics. That was a big deficit. Nonetheless, it’s a major structure across the country that allowed for the fight against the pandemic.
I work in a federal institution, the Fiocruz Foundation, the biggest federal health body in the country. We have the capacity to produce important research, we work on national projects and we have several international partners. We are able to produce medications for endemic diseases, malaria, tuberculosis, and also vaccines. Fiocruz and Intituto Butantan are the two public institutions in Latin America capable of producing vaccines. We offer SUS 16 types of vaccines for the Brazilian people: chicken pox, measles, flu shots, all the vaccines for the children and for the elderly.
It’s important to understand all this because this is the structure that — to a certain extent — kept the pandemic at bay. But we weren’t able to use SUS’s whole potential. For instance, we could have prevented many deaths that happened at home because of an initial mistake by the government and the WHO. They said that people shouldn’t seek out medical attention unless it was a serious case. If, for instance, we had optimized telemedicine — which we are doing right now — people could have used their cell phone to have contact with doctors and nurses. Perhaps we could avoid many deaths, but this wasn’t done adequately.
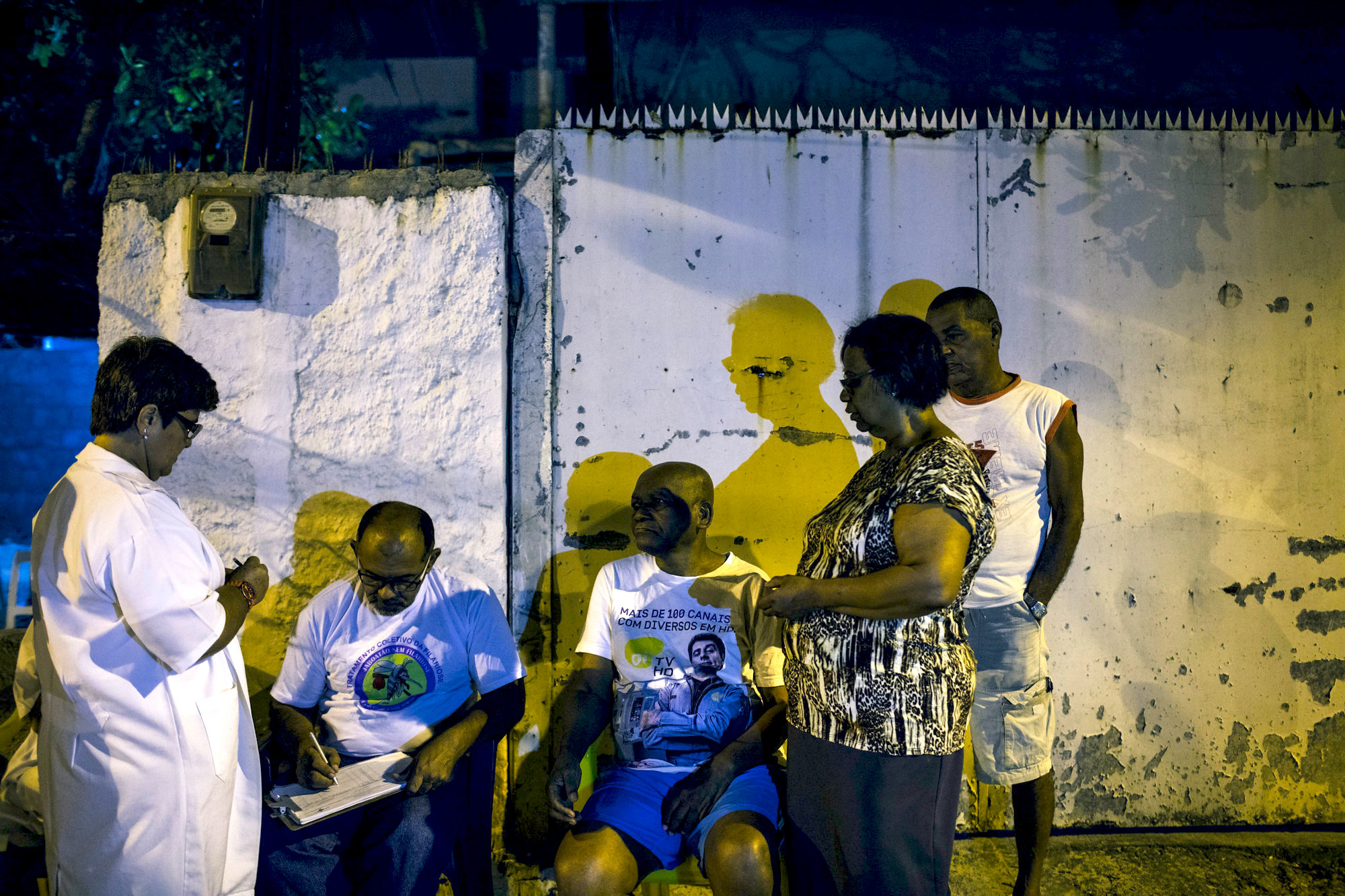
2015: Brazilians receiving the microfilaria test, which must be conducted between 11 pm and 1 am, outside a bar in Jaboatão dos Guararapes, Pernambuco. (Pan American Health Organization, Flickr, CC BY-NC 2.0)
You’ve raised a very important point since Brazil’s President Jair Bolsonaro used to say that strict measures against the virus are not viable economically. That is of course cynical, but the growth of poverty is a real problem. We just published a study that showed there are 19 million people suffering from hunger in Brazil. What measures should be adopted given this economic situation?
Without a doubt, we need to overcome the discussion that sees a dichotomy between the economy and health. To control the pandemic right now, we need social distancing and mass vaccination. To be able to have this, we need to keep people at home. How can we keep people at home? It’s easy for middle-class people, for my family, for your family. But for people who live in poor neighborhoods, it’s not easy. They live mostly off the informal economy.
When the first wave hit, it was clear to us what needed to happen: the government should have started to supply the so-called emergency aid to keep low-income people afloat. It was clear that if we didn’t assist these people the situation would become much more tragic. Brazil is a country with an unacceptably high-income concentration. The difference between the haves and have-nots is just unbelievable.
“The government should have started to supply the so-called emergency aid to keep low-income people afloat.”
But it quickly became clear that there wouldn’t be enough emergency aid from the government because it was seen as an economic measure. I have repeatedly said that there’s no dichotomy between health and the economy — it’s the same thing. To give aid for people who have no income is a public health measure, not an economic one. If people in Brazil have to decide between dying of hunger or dying from the virus, that’s just not acceptable.
To give aid for people who have no income is a public health measure, not an economic one.
At some point, the emergency aid that the government gave during five or six months ran out. It has been reactivated this month but with a much lower amount. At first, it was around €100, now it’s less than half. That’s not even enough for food for one month.
In Sao Paulo, the biggest hospital network, all the beds are full. There are lines, people waiting to be admitted. In Rio de Janeiro and other state capitals it is the same. The situation we are undergoing right now is as acute as during the peak in the middle of the last year. But it’s worse because of the social factor, the tiredness of people vis-à-vis a pandemic that has lasted more than a year.
What are your expectations of the international community to make sure that more vaccines reach the country and the region? What do you think about the proposal to waive vaccine-related patents?
Right now, we are in a difficult situation because there are no vaccines for sale. Brazil has signed up to the WHO’s COVAX facility and we negotiated vaccines for only 10 percent of the population. That was a mistake, we should have negotiated 30 or 40 percent through COVAX. On top of that, we have not yet received a single vaccine from COVAX. Why? Look at Europe.
The international systems don’t work well enough. The Covid-19 pandemic actually revealed their obscenity. The social inequality globally is just scandalous. If 10 countries buy up 75 percent of all the global production of vaccine in 2021, that’s scandalous. But in Portugal, Germany, France, it’s also a catastrophe. In France, for instance, they have plenty of vaccines but they don’t have the agility Brazil would have to vaccinate.
“The social inequality globally is just scandalous.”
Having said all that, the international community can help. To give you a simple example: the U.S. has millions of doses of the AstraZeneca vaccine that they are not using because the FDA has not approved it. So it’s fundamental for Brazil to negotiate a donation of these surplus vaccines. We understand that the U.S. is going to vaccinate their own population first. But they are not using the AstraZeneca vaccine —and we are. We could be negotiating that right now.
On the question of patents: Brazil has been in discussion with the WHO about this. Of course, Brazil has experience with breaking patents for anti-retroviral drugs against HIV/AIDS, which made it easier to conduct a top-quality national AIDS program. So, I’m not only in favor of the discussion, but of actually breaking the patents. However, that will not solve today’s problems. Even if we are able to break the patents, it takes time to ramp up manufacturing. It’s not an easy, quick process. This will be a solution for next year, it’s not a solution for the immediate future when we need to improve the rollout.
Right now there are discussions of the private sector in Brazil buying vaccines. How do you evaluate the role of the private sector?
Right now we need to vaccinate a lot of people and very quickly. Brazil is a huge country. There are regions that are difficult to access and here the private sector can help. We are however against the purchasing of vaccines by the private sector, it has to be done institutionally. As it’s set out in the constitution, SUS has to be the purchaser.
But what the private sector can do is to finance the logistics. We have asked all the municipalities in Brazil and received a 99 percent response rate on what they need. There are municipalities that need a plane, a plane that can land in small landing strips, others need refrigerators, freezers, computers, thermal boxes, motorbikes, boats. All of this is being organized in a good way. But we need the vaccines, that’s the problem we need to solve.
How optimistic are you that we can still achieve international solidarity when it comes to the pandemic?
There’s no way around it. The international community has to review aged concepts. Covid-19 is a phenomenon that has changed our lives. I often say that it is like AC and BC: we live in a world defined by After Covid and Before Covid, and nothing will be the same again. It’s not like other viruses, like H1N1. We were able to contain that, produced a vaccine, and vaccinate everyone every year. SARS Covid-2 will not disappear, it will stay endemic. There will have to be vaccines and the vaccines will have to be improved and enhanced. The current wave of vaccines are just first-generation vaccines. Very quickly there will be new generations that will cover the variants that are appearing, particularly the messenger-RNA vaccines that are very easy to recompose.
But that aside, we need to have a different way of looking at the world. Covid-19 induced mortality has a social component that cannot be ignored — people are dying because they are poor. Even in a rich city like New York, 40 percent of the deaths were poor and Black people. This is unbearable. In Brazil, the death rates in poor communities will be much higher than among the middle and upper-class people. This requires a new quality of solidarity, domestically and internationally.
I have no doubt that the world demands it: the academics, the philosophers, the intellectuals, the community leaders, the faith communities need to be linked in this discussion. Covid-19 is a phenomenon that has changed our lives, but also served to bring some kind of hope for a new quality of solidarity.
Margareth Dalcolmo is a pulmonologist and researcher at the Oswaldo Cruz Foundation, one of the most important health bodies in Brazil, with experience in conducting and participating in protocols for clinical research and treatment of tuberculosis and other mycobacterioses. She is a member of the Advisory Committee on Tuberculosis of the Ministry of Health. She is also a member of the WHO Expert Group for Essential Medicines List and the World Bank Regional Advisory Committee for health projects in Sub-Saharan Africa on Tuberculosis and occupational respiratory diseases.
This interview was conducted and edited by Christoph Heuser and Daniel Kopp.
This article is from International Politics and Society.
The views expressed in this interview may or may not reflect those of Consortium News.


